“Of all the forms of inequality, injustice in health care is the most shocking and inhumane.” – Martin Luther King
SOUTH AFRICA SUFFERS FROM AN enormous burden of disease and ill health that affects all of us. It affects us as individuals. But it also affects us as a racialised, unequal, broken society divided along multiple fracture lines, such as wealth, geography, and level of education.
Our divided health system reproduces and deepens these social ills. On the one hand, we have a public sector that anyone can use. But it is crippled by austerity and poor management. On the other, a mercenary private sector services the elite 16% of the population that belongs to medical aid schemes, together with a smaller number of relatively rich people who can pay for care out of pocket.
This system is massively unequal. It operates according to the Inverse Care Law:
The availability of good medical care tends to vary inversely with the need for it in the population served. This inverse care law operates more completely where medical care is most exposed to market forces, and less so where such exposure is reduced.
The government aims to fix this by establishing National Health Insurance. The NHI Bill was passed by parliament; it still has to be approved by the National Council of Provinces before it goes for the President’s signature. The Bill sets up a fund, called the National Health Insurance Fund (NHIF), “as the single purchaser and single payer of health care services, in order to ensure the equitable and fair distribution and use of health care services”.
Single-payer health system
In a single-payer system, one entity – for example the NHIF – collects all the money for health care and pays for everyone’s health care costs. Everyone pays into the fund according to how rich they are. Those who live in poverty and don’t have the means don’t have to pay. But everyone, rich and poor, has fair, equitable access to the healthcare they need. The wealthy support the poor, the healthy support the sick, and the young support the elderly. In this way, we reduce inequality and come closer together as a nation.
Single-payer systems are more efficient and less costly than multiple-payer systems. They make it possible — but do not guarantee — to deliver health care equitably according to need rather than means. Importantly, and very relevant for the NHI, for the benefits of the single-payer to materialise, the system must be implemented well and with complete transparency and accountability to the users. This is in line with the state’s constitutional obligation as a duty-bearer to provide health care to everyone as a human right, as specified in section 27 of the constitution.
However, many people don’t trust the process, and the NHI project is highly controversial. At its heart, the dispute is between private interests and the public good. Much of the controversy amounts to mere fear-mongering by groups who fear losing the privileges of the current system: “It will destroy the health system!”, they say. “We already pay too much tax! Doctors will emigrate in droves! Where will the money come from?”
Other concerns are more substantial, including from progressive groupings. Can the NHI achieve what it intends? Will it deliver equitable Universal Health Coverage that delivers health care to all according to need? Will it promote equality, social solidarity and justice? How will the NHIF be protected from corruption?
The finance controversy

“Lady Grey Hospital E.Cape. On the one hand, we have a public sector that anyone can use. But it is crippled by austerity and poor management.”
Public submissions on the NHI Bill express almost unanimous support for the principle of Universal Health Coverage (UHC). The main controversy rages over the NHI as the implementing mechanism.
The Bill stipulates that it will fund progress towards Universal Health Coverage (UHC). According to the World Health Organisation, Universal Health Coverage (UHC) means that all people and communities have access to the promotive, preventive, curative, rehabilitative, and palliative health services they need. They have that access where and when they need them (equitable). The services are of sufficient quality (effective). And using them does not expose them to financial hardship (affordable).
However, as Joseph Kutzin, Coordinator for Health Financing Policy at the WHO, points out, this formulation is open to a range of interpretations that can be used to advance specific interests. In the case of the NHI, this boils down to a choice between two radically different interpretations of UHC:
- A rights-based, universal, publicly funded, tax-based, single-payer system. This harnesses all available resources to provide equitable health care to the population as a whole, or
- A multi-tiered, insurance-based, private system that provides cover for members of schemes. This would possibly have some private-public partnership arrangements in places. But it would largely run separately, in parallel to an improved public sector providing care to the poor.
It goes without saying that our UHC model must embody the specific goals of the NHI project and of our health system as a whole.
The goals of the NHI are laid out in the Government Gazette of 11 September 2009: The introduction of a National Health Insurance System is founded on three principles. Firstly, that it is a Constitutional right that the public has access to affordable and acceptable quality health services; secondly, that it is the responsibility of the State to ensure the progressive realisation of the right to health for all South Africans that is premised on the objective of universal coverage; and thirdly, that it is important for health services to be funded in an equitable manner that promotes social solidarity”. – (Department of Health 2009)
The central goal of the health system can only be to ensure that everyone can enjoy their highest possible level of health, whatever their context (for example, their level of income, education, underlying health conditions and so on).
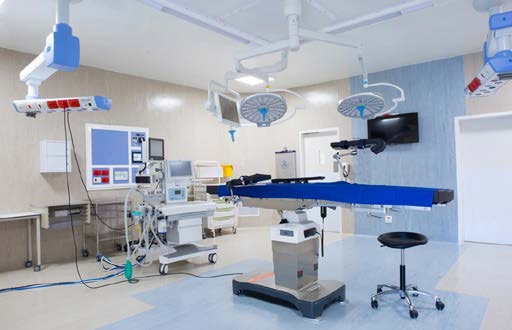
Mediclinic Stellenbosch. We have a mercenary private sector that services the elite 16% of the population that belongs to medical aid schemes, together with a smaller number of relatively rich people who can pay for care out of pocket.
International evidence overwhelmingly favours publicly-funded, tax-based systems over insurance scheme-based models. Apart from being less costly, they have other social and economic benefits beyond quality health care. Here is some of the evidence:
- Single-payer systems tend to be less costly than multi-payer systems in a number of ways. A systematic review of economic analyses in the United States found that single-payer systems would reduce health expenditures while providing high-quality cover to all residents through simplified billing, negotiated drug price reductions, and global budgets to control spending growth over time.
-
Economic growth is not a necessary prerequisite for starting to move towards UHC. This was shown in a study of 11 countries attempting to move towards UHC and published in The Lancet in 2015. UHC needs cross-subsidisation from the rich to the poor, and from low-risk groups (e.g., the young) to high-risk groups (e.g., the elderly). Social movements in civil society play a catalytic role in putting UHC on the political agenda and encouraging governments to face opposition and implement meaningful change — strong political will to confront groups with vested interests is essential.
-
Single-payer systems have beneficial effects beyond better and more equitable healthcare delivery and cheaper drugs. In February 2022, the US Congressional Budget Office (CBO) reported on a study of the economic effects of five single-payer health systems. They found that with these systems, although GDP could fall by between approximately one and ten per cent by 2030, this would be offset by growth in economy-wide productivity. There would be more jobs and less unemployment. Workers would enjoy higher wages and pay lower insurance premiums and out-of-pocket expenses. Disposable household income would increase, leading to more savings. Workers would choose to work fewer hours, and families would have more time for activities outside their paid work.
-
Multiple-payer systems make UHC more difficult to achieve. This is because voluntary insurance schemes benefit some people at the expense of the rest of the population and the system as a whole. They also set up groups in society with unequal risks, benefits and economic power, who resist further change that might threaten their position. Their interests conflict with the aims of UHC to benefit the system as a whole.
The Hospital Association of South Africa, the main private hospital grouping, knows that public service models are cheaper. But it continues to promote the more costly, insurance scheme-based model. Their own Econex study found that public service-type models provided greater access or higher levels of coverage at lower costs than insurance-based models. High administration costs contributed to insurance-based models “being more expensive than systems where healthcare is funded through taxation and provided as a public good”.
Yet, HASA’s submission to parliament argued in favour of insurance-based models. They ignored the Econex report because its findings did not serve their interests. This is a prime example of how the finance controversy is manufactured to protect vested commercial interests in the private sector.
From the evidence, it is clear that the single-payer system based on tax is the appropriate option for the NHI. It is also in line with the Bill of Rights and the principles expressed in the original Government Gazette. Pooling the funds from those who have the means to pay for health care for everyone is essential for social solidarity. It means we all pull together to heal the nation.
Why the NHI is likely to fall short — at least this time round
Despite all the good intentions and ideals behind the NHI project, it is very likely to fall short of meeting its aims. The South African state is too dysfunctional and derailed by corruption, poor, unaccountable governance, and lack of political will to make it happen.
Progressive organisations that support the idea of the NHI and campaign passionately for health for all and a unified public health service made submissions to parliament’s Portfolio Committee on Health. They expressed serious and justified concerns about the possibility that the NHIF will be plundered through corruption. These organisations include the People’s Health Movement, the Treatment Action Campaign, Section 27, and the Health Justice Initiative.
Collaboration for Health Systems Analysis and Innovation, based at UCT and UWC, made a submission. It says unequivocally that “experience makes clear that the threat of corruption and misuse of health funds is a very real threat to the NHI and therefore to the health and well-being of everyone living in South Africa”. There were many other submissions that expressed similar concerns and outright scepticism about corruption, poor governance, and lack of adequate provision for accountability and control.
Instead of a unitary National Health Service that makes good health care easily accessible according to need rather than means, the current NHI project is likely to deliver a still fragmented and unequal, multi-tiered health system that does not do away with the inverse care law.
The Achilles heel of the NHI project lies in the failure of the state to implement a good policy because of endemic corruption, poor governance and lack of accountability. The NHIF is set up as an insurance fund rather than a National Health Fund. We have seen the shortcomings of the insurance model. To progress towards universal health care, the state will have to counter powerful opposition from organisations with vested interests in profitable private health care, as well as neoliberal libertarian think tanks like the Institute of Race Relations and the Free Market Foundation. It will also have to root out corruption. And, fundamentally, it will have to gain the trust of the nation. Sadly, none of this seems to be happening with any urgency.
What is to be done?

Despite all the good intentions and ideals behind the NHI project, it is very likely to fall short of meeting its aims. The South African state is too dysfunctional and derailed by corruption, poor, unaccountable governance, and lack of political will to make it happen.
The real question around the NHI is whether it will result in the establishment of a united, equitable National Health Service that can make good quality essential healthcare easily accessible to all, according to need.
Progress towards health for all requires active citizenship, mobilisation towards shared values, and a vision of the kind of country we want our children and grandchildren to live and grow up in. We can’t leave this to the state, the private sector or the market.
The state can’t do it and the powerful private sector opposes it. This means it is up to us, the people, to continue the struggle for health. We have to rescue the NHI from privatisation under neoliberal, free market, fundamentalist ideology. And we need to ensure that it follows a human rights approach that belongs to all.
Such an approach is fundamental to health services that provide good health care equitably, according to need rather than wealth, status, station in life, or other factors that put some people in positions of power. Unlike access based on medical scheme cover, human rights are universal. They belong to all of us, everywhere; they are inalienable – no one can take them away from us, and they are indivisible – they are all interconnected and interdependent.
It’s important to bear in mind that even the best health service is not enough to ensure health for all. For that, we have to ensure that everyone enjoys access to the goods and services and an environment and working conditions that promote health. These include adequate housing, good education, food security, safe environments, personal safety and security, transport, water and sanitation. They are generally known as the social determinants of health (SDH), but they are also political and economic.
Access to the SDH involves state sectors other than the health sector. This means that virtually all struggles are also health struggles.
Louis Reynolds is a member of the People’s Health Movement of South Africa. He writes in his personal capacity.

0 Comments